 Author :
Dr. Sheikh Jeelani
/
BNYS | FTECH
Author :
Dr. Sheikh Jeelani
/
BNYS | FTECH
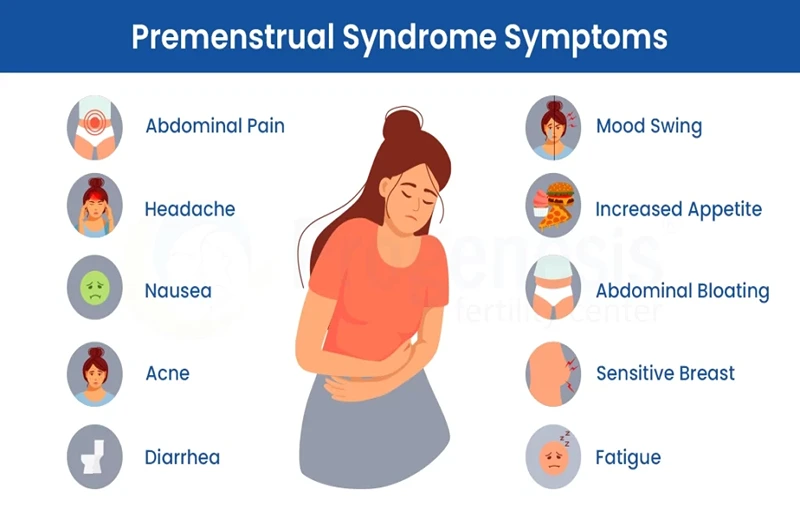
What is Premenstrual Syndrome (PMS)?
Premenstrual syndrome refers to a group of physical, emotional, and behavioural symptoms that occur in the days leading up to a period. These symptoms usually appear during the second half of the menstrual cycle, after ovulation, and often ease once the period begins. PMS is believed to be linked to the natural hormonal changes that take place during this phase, particularly shifts in oestrogen and progesterone levels.
PMS affects each person differently. For some, the symptoms are mild and barely noticeable. For others, they may be more pronounced and interfere with daily activities, relationships, or general wellbeing. The severity and type of symptoms can also vary from cycle to cycle. Although PMS is common, it is not something that has to be endured in silence. With the right awareness and approach, its effects can often be recognised and managed effectively.
What Causes PMS?
The exact cause of PMS is not fully known, but it is mainly linked to hormonal changes during the menstrual cycle. After ovulation, levels of oestrogen and progesterone rise and then drop sharply if pregnancy does not occur. This shift can affect certain brain chemicals, such as serotonin, which influence mood, sleep, and appetite. As a result, emotional and physical symptoms associated with PMS may appear in the days before a period begins.
Other factors can also make PMS symptoms more noticeable. These may include high stress levels, poor sleep, lack of exercise, and a diet low in essential nutrients. Some people may also be more sensitive to these hormonal changes than others, which could explain why PMS varies so widely from person to person.
Frequently Asked Questions
Q1: Can PMS symptoms change as a person gets older?
A1: Yes, PMS symptoms can shift with age. Some people experience more noticeable symptoms in their 30s and 40s, especially as hormonal patterns begin to change in the years leading up to menopause. These changes may include stronger mood swings, heavier bloating, or increased breast tenderness. Tracking symptoms across cycles can help detect any changes early and guide discussions with a gynaecologist.
Q2: Does hormonal birth control have any effect on PMS?
A2: Hormonal birth control can sometimes reduce PMS symptoms by preventing ovulation and stabilising hormone levels throughout the cycle. In some cases, it may also change the pattern of symptoms or cause side effects of its own. The response to birth control varies from person to person, so it’s best to discuss options with a doctor who can recommend the most suitable method based on individual needs.
Q3: Is it possible to experience PMS after menopause?
A3: No, PMS only occurs in people who are still ovulating. Once menopause is reached and periods stop, PMS symptoms should no longer appear. However, the hormonal changes that occur during menopause may cause symptoms that feel similar to PMS, such as mood changes or disrupted sleep, though these are related to a different phase of hormonal transition.
Q4: How is PMS different from PMDD?
A4: PMS and PMDD both involve physical and emotional symptoms in the days before a period, but PMDD (premenstrual dysphoric disorder) is more severe. It causes intense mood changes, such as extreme irritability, sadness, or tension, and can significantly interfere with daily functioning. PMDD usually requires medical treatment and ongoing support.
Q5: Can PMS cause digestive issues or changes in appetite?
A5: Yes, many people notice digestive symptoms like bloating, constipation, or even loose stools in the days before their period. Appetite changes are also common and may include cravings for salty or sugary foods, or feeling hungrier than usual. These symptoms are linked to hormonal shifts that affect digestion and metabolism during the premenstrual phase.
Q6: Are there medical treatments available if lifestyle changes don’t work?
A6: If PMS symptoms continue to disrupt everyday life despite home-based strategies, medical treatment may be considered. Options can include hormonal therapy, non-hormonal medication, or treatments that target specific symptoms such as mood or pain. A gynaecologist will usually recommend a detailed assessment before suggesting the next step.
Q7: Can PMS-like symptoms sometimes point to another health condition?
A7: Yes, symptoms that resemble PMS can occasionally be linked to other conditions, such as thyroid disorders, endometriosis, or mood-related conditions like depression or anxiety. If the timing, intensity, or nature of symptoms changes suddenly, or if they appear outside the typical premenstrual window, it is worth seeking a medical opinion.
Q8: Does PMS affect the ability to conceive?
A8: PMS itself does not impact fertility. It occurs during regular menstrual cycles and is not a sign of fertility problems. However, if the symptoms are caused by another condition like polycystic ovary syndrome (PCOS) or endometriosis, then fertility may be affected. In such cases, early diagnosis and treatment can help support future reproductive plans.